 Do you have a space where a tooth used to be? Were you born with a missing tooth? Are you getting ready for dentures? You may be a good candidate
Read more
Do you have a space where a tooth used to be? Were you born with a missing tooth? Are you getting ready for dentures? You may be a good candidate
Read more
-
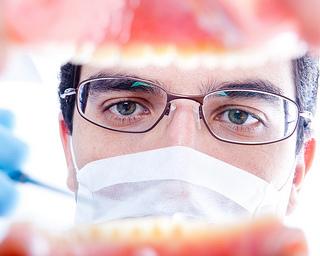
What are dental implants?
posted: Apr. 23, 2024.
 Do you have a space where a tooth used to be? Were you born with a missing tooth? Are you getting ready for dentures? You may be a good candidate
Read more
Do you have a space where a tooth used to be? Were you born with a missing tooth? Are you getting ready for dentures? You may be a good candidate
Read more
-
Make Every Day Earth Day
posted: Apr. 16, 2024.
 Earth Day began in 1970 as an event to raise awareness of our environment. What began as a single day in April is now recognized around the world to bring
Read more
Earth Day began in 1970 as an event to raise awareness of our environment. What began as a single day in April is now recognized around the world to bring
Read more
-
Why Baby Teeth Matter
posted: Apr. 09, 2024.
 Sleepless nights, crankiness, drooling—how can such tiny teeth cause such a big fuss? But all those uncomfortable days and nights are forgotten when your baby’s first teeth make their appearance.
Read more
Sleepless nights, crankiness, drooling—how can such tiny teeth cause such a big fuss? But all those uncomfortable days and nights are forgotten when your baby’s first teeth make their appearance.
Read more
-
Oral Cancer Awareness Month
posted: Apr. 02, 2024.
 Happy Oral Cancer Awareness Month! We know oral cancer can be kind of a scary topic, but it’s worth using this opportunity to learn about the disease and spread knowledge
Read more
Happy Oral Cancer Awareness Month! We know oral cancer can be kind of a scary topic, but it’s worth using this opportunity to learn about the disease and spread knowledge
Read more
-
Water: It’s Not Just for Brushing!
posted: Mar. 26, 2024.
 We turn on the tap and it comes rushing out. We walk down the hall at work or school and stop at the fountain without even thinking about it. It’s
Read more
We turn on the tap and it comes rushing out. We walk down the hall at work or school and stop at the fountain without even thinking about it. It’s
Read more
-
Quit Smoking to Save Your Smile
posted: Mar. 19, 2024.
 You’ve likely heard that smoking increases risk of lung cancer and emphysema. But did you realize that your cigarette habit also has an impact on your smile? Chronic smokers suffer
Read more
You’ve likely heard that smoking increases risk of lung cancer and emphysema. But did you realize that your cigarette habit also has an impact on your smile? Chronic smokers suffer
Read more
-
St. Patrick's Day: Celtic pride, green shamrocks, and lucky charms!
posted: Mar. 12, 2024.
 “St. Patrick's Day is an enchanted time -- a day to begin transforming winter's dreams into summer's magic.” Adrienne Cook
Lucky green shamrocks, leprechauns, and pots of gold – it must
Read more
“St. Patrick's Day is an enchanted time -- a day to begin transforming winter's dreams into summer's magic.” Adrienne Cook
Lucky green shamrocks, leprechauns, and pots of gold – it must
Read more
-
March is National Nutrition Month!
posted: Mar. 05, 2024.
 While you don’t have to wait to start eating right, March is the month the Academy of Nutrition and Dietetics asks everyone to pay special attention to what goes into
Read more
While you don’t have to wait to start eating right, March is the month the Academy of Nutrition and Dietetics asks everyone to pay special attention to what goes into
Read more
-
Tips for Managing Oral Pain
posted: Feb. 27, 2024.
 Experiencing tooth or oral pain is not fun. If you cannot get to Tressa Priehs DDS right away, the pain may even seem to increase. The old saying that a
Read more
Experiencing tooth or oral pain is not fun. If you cannot get to Tressa Priehs DDS right away, the pain may even seem to increase. The old saying that a
Read more
-
Dental Sealants for Baby Teeth?
posted: Feb. 20, 2024.
 Perhaps you’ve heard your friends talking about dental sealants, and how well they prevent cavities. And as soon as your child’s permanent molars come in, you absolutely plan to make
Read more
Perhaps you’ve heard your friends talking about dental sealants, and how well they prevent cavities. And as soon as your child’s permanent molars come in, you absolutely plan to make
Read more
-
Team Dark Chocolate
posted: Feb. 13, 2024.
 Valentine’s Day is the holiday to celebrate all the treasured relationships in your life. It’s a time to honor love in all shapes and forms with cards, social gatherings, and
Read more
Valentine’s Day is the holiday to celebrate all the treasured relationships in your life. It’s a time to honor love in all shapes and forms with cards, social gatherings, and
Read more
-
Warning Signs of Impacted Wisdom Teeth
posted: Feb. 06, 2024.
 You might suspect that your wisdom teeth are starting to emerge, but knowing the signs of impacted wisdom teeth can help you be more proactive about your dental care. Impacted
Read more
You might suspect that your wisdom teeth are starting to emerge, but knowing the signs of impacted wisdom teeth can help you be more proactive about your dental care. Impacted
Read more
-
Camping Oral Health Tips
posted: Jan. 30, 2024.
 If your idea of camping is a quiet walk through the woods before returning to your rustic hotel, your regular brushing habits will be perfect for your trip. But if
Read more
If your idea of camping is a quiet walk through the woods before returning to your rustic hotel, your regular brushing habits will be perfect for your trip. But if
Read more
-
What are dental crowns?
posted: Jan. 23, 2024.
 A dental crown is often called a “cap.” A dental crown covers all of the visible parts of the tooth and has many functions and reasons for placement.
There are several
Read more
A dental crown is often called a “cap.” A dental crown covers all of the visible parts of the tooth and has many functions and reasons for placement.
There are several
Read more
-
Root Canal Recovery
posted: Jan. 16, 2024.
 Anyone who has had a compromised tooth knows that the amount of discomfort it causes can be extremely unpleasant. Although no one looks forward to a root canal, this procedure
Read more
Anyone who has had a compromised tooth knows that the amount of discomfort it causes can be extremely unpleasant. Although no one looks forward to a root canal, this procedure
Read more
-
Diabetes and Dental Care
posted: Jan. 09, 2024.
 Diabetes is a disease that affects the health of the entire body, including, of course, your mouth, gums, and teeth. We are trained to look for issues that might arise
Read more
Diabetes is a disease that affects the health of the entire body, including, of course, your mouth, gums, and teeth. We are trained to look for issues that might arise
Read more
Contact Us
Office Hours
Monday:
10:00 am - 7:00 pm
Tuesday:
7:00 am - 5:00 pm
Wednesday:
7:00 am - 4:00 pm
Thursday:
7:00 am - 2:00 pm
Friday - Sunday:
Closed
